Qualifying for Surgery
We are excited to announce that based on the latest 2022 ASMBS/IFSO criteria, we can now offer bariatric surgery to individuals with Body Mass Index > 30. Candidates include those with 30-40 lbs over ideal body weight and any of the obesity-related conditions such as diabetes or pre-diabetes, obstructive sleep apnea, high blood pressure, high cholesterol, joint disease, acid reflux, low back pain, etc. Surgery can also be offered to individuals with BMI > 35 without co-morbidities listed above. These new criteria allow access to life-saving procedures to millions of individuals who were previously excluded under the 1991 NIH consensus conference criteria.
Bariatric surgery is suitable for motivated individuals who have genuinely tried to lose weight through dieting and exercise but have failed to maintain a healthy weight. To determine if your excess weight is sufficient to qualify you for surgery, your Body Mass Index (BMI) is used. BMI is the ratio of your weight in kilograms, over your height in meters to the power of two (BMI=Kg/m2).
To determine your BMI, use the BMI calculator below.
-
Less than 19UNDERWEIGHT: You are under optimum weight for your height. You could afford to gain a little weight.
-
20 - 24.9ACCEPTABLE: You have a healthy weight for your height.
-
25 - 29.9OVERWEIGHT: You are over optimum weight for your height. You may be facing health problems, so losing some weight would be a good idea.
-
30 - 34.9OBESE: You are over optimum weight for your height and face increased risks to your health. Most likely you qualify for bariatric surgery.
-
> 35SEVERELY OBESE: You are over optimum weight for your height and your excess weight can cause severe health problems. You qualify for bariatric surgery.
In addition to your BMI and medical conditions, Dr. Zaré will review other pertinent information in determining whether you are a suitable candidate for surgery. For you to achieve maximal success after surgery, it is essential to understand exactly how bariatric surgery works and what changes to lifestyle are necessary. Our program will provide you the necessary education and support and help you reach you goal efficiently.
After you decides to proceed with surgery, there are two possible pathways to surgery. You can either use insurance coverage to share in the cost of the surgery, or elect to finance the procedure yourself.
Many insurance plans provide bariatric benefits and may be used to cover parts of the cost the procedure. The steps involved in using your health plan for coverage of bariatric surgery can be broken down to the following 5 steps.
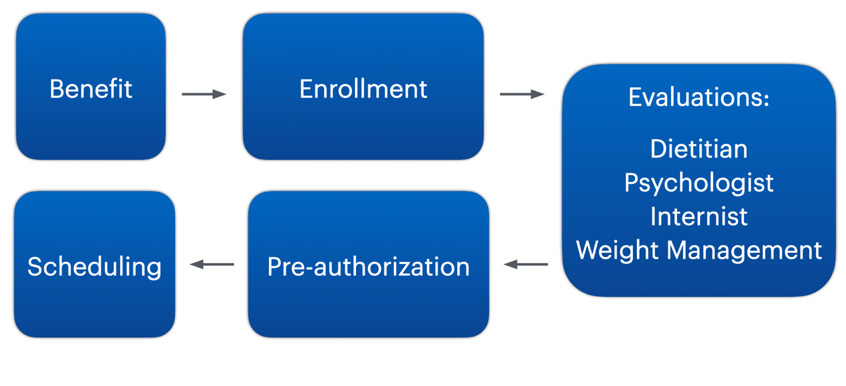
The first step in this process is to confirm that your policy includes bariatric surgery benefits. You may do so by contacting your health plan and providing them the CPT code 43775 for Laparoscopic Vertical Sleeve Gastrectomy. Once benefits are confirmed, you can enroll in our program and proceed with obtaining necessary evaluations and other insurance requirements. A complete list of requirements will be provided to you at your first consultation. This information may also be obtained from your health plan. Typical requirements include assessments by registered dietitians, mental health specialists, medical specialists, etc. Health plans may also require your participation in a medically supervised weight-loss program lasting 3-6 months within a year of planned surgery. Once complete, a pre-authorization will be obtained, and surgery scheduled. It can take between 2-9 months to complete an insurance pre-authorization process. Our program will help you determine and fulfill these requirements prior to surgery.
Many individuals choose to self-finance their procedure and forego the process of insurance pre-authorization. These include individuals with BMI 30-34.9, individuals with no insurance coverage, individuals with coverage but without bariatric benefits, or simply individuals interested in expedited care. For these individuals, the self-financed process typically takes 3 weeks to complete.
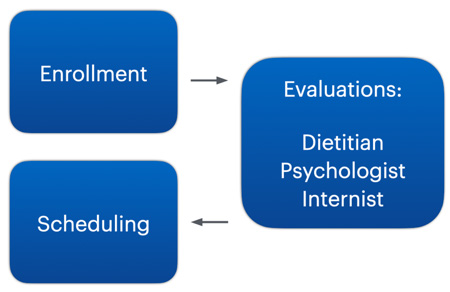
Financing is available. For additional information about this pathway, please click here.